
Compassionate Care at cCARE: What Patients Should Know
At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.
Monday, January 19, 2026 – Closed
In observance of Martin Luther King Jr. Day.
I’m Joel Lamon and I’m a medical oncologist at cCARE. It’s important to know that testicular cancer is the most common cancer in American Caucasian males below the age of 40. And I don’t think there’s a better age group for having a malignancy and being associated with denial about symptoms than in that age group and gender.
So many times when a cancer is diagnosed it’s advanced. Sometimes young men will come to the doctor because they feel a hard mass in the testicle. Many times, it’s after an apparent sports injury, where they are playing sports and they notice this, thinking they may have hit themselves or been injured that way. And often it’s not the case.
So, concerns are that advanced cancers are not survivable and secondly that male fertility may be lost in treatment of testicular cancer. Both are inaccurate. A lump in the testicle is something that can bring a young man or a young adult to a doctor’s attention, and often it’s because they were in a sports injury, or some incidental injury-type situation and they think the cancer has been affected. Other times it can be abdominal or back pain, cough or chest pains.
In some advanced cancers where there are brain metastases, symptoms might affect brain function. The testes are typically asymptomatic, but infections of the testes can present as a swelling, a mass. Usually there’s inflammation, where in testicular cancer that’s not the case. But any mass or swelling or discomfort in the genitals is certainly a cause for alarm.
There are family cases of testicular cancer. But it is not considered an inherited cancer. It’s certainly reasonable to have self-exams for testicular cancer, and in the very age group I mentioned, to the age of 40. It’s not something that is a common enough disease as in breast cancer to recommend routine self-exams.
However having awareness in the young male population, as I mentioned that this is a potential malignancy, I think that any asymmetry in the testes – remembering that they’re about two centimeters in length and they should be similar in size although our bodies are somewhat asymmetric – so any hard mass in the testes should call attention to that individual to seek physician evaluation.
There is no specific risk factor that I can share with you. As I said, there may be some misconceptions that certain activities have led to testicular cancer, when in fact it’s typically coincidence.
There have been significant breakthroughs in treatment of testicular cancer over the past 40 years. It’s considered a curable disease. If the cancer is isolated to the testes, surgery is a curative treatment. But it’s remarkable to say that even with distant spread of disease, that is disease that may be in the chest or even the brain, testicular cancer is curable. I can’t make that as a 100% blanket statement, but it is a high enough percentage that every individual should be seen by a medical oncologist to evaluate options for treatment.
Testicular cancer occurs in one teste or the other and it spreads as any cancer might by blood and lymphatic channels. So, in the evaluation of a testicular mass, many times a sound wave of a testicle will clearly identify whether this is a cyst or an infection or a solid tumor mass. Imaging studies will help us know if there are regional lymph nodes, that is lymph nodes in the groin or in the back of the abdomen.
And of course, full staging is important, and an oncology evaluation would undertake that to look through the full extent of the body for any signs of disease. We’re also helped in many, but not all testicular cancers, in having tumor markers, and what I mean by that is that these are proteins in the blood that are associated with the type of germ cell in the testes, and that can be very helpful in knowing if there is a significant tumor mass and very helpful in knowing the success of treatment.
Testicular cancer if localized can be treated by surgery. There are some specific forms of testicular cancer that may be best suited for radiation treatment. But many cancers, especially if they have spread beyond the testes and are in the abdominal or chest cavities, are treated with chemotherapy.
I would say we are not treating children with testicular cancer we’re treating young adults, adolescents and beyond once the testes have matured. In treatment of testicular cancer, it’s very frequent that the testes that’s affected is removed by surgery as part of the plan for treatment and evaluation.
Men can be fertile with one testes. Fertility does vary with the sperm count. And the sperm count will go down with removal of testes and it will go down for a period of time after chemotherapy. And so, hypofertility [abnormally reduced fertility] may in fact be the case in some men for several years post treatment.
Sperm banking is certainly a possibility and can be done for a man with testicular cancer. This may be occurring in a man in childbearing years and he may be concerned that hypofertility is a potential limiting factor in having a family. But it should not be viewed that having testicular cancer or losing one testes eliminates the ability to father a child.
What would limit sexual activity after surgery or chemotherapy is any individual’s vigor, that is recovering from surgery, recovering from chemotherapy. The most significant issue is for a partner in sexual activity: would there be any chance of exposure to the partner from any chemotherapy that might be in the semen? That certainly is possible that chemotherapy drugs are in semen, but they would not be there permanently and it’s usually short lived. I think it’s best discussed with your physician with regard to your sexual activity and protection of your partner, if that’s something that is desired during the course of treatment.
cCARE holds a body of knowledge that’s common throughout western medicine. cCARE offers, in my opinion, nothing more that would be offered anywhere else. But more importantly cCARE offers nothing less than is offered anywhere else including university systems. Our physicians are all university trained, the drugs are available to all of us, and we understand the importance of chemotherapy for advanced disease. Radiation facilities are available to us in our offices or in our communities. If in fact cCARE radiation is not possible due to insurance coverage, our state-of-the-art services are duplicated in many places throughout the country.
I think what’s important is not the technology, not the bricks and mortar that we bring, but it’s our compassion and sharing our intellect with our patients in a way that allows them to have success in treatment that goes beyond just the biology.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.
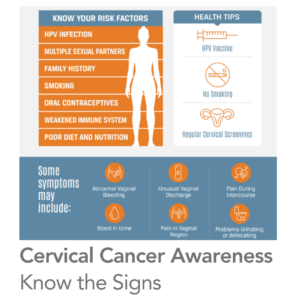
In early stages, cervical cancer may not cause noticeable symptoms. As it progresses, some signs may include: