
Compassionate Care at cCARE: What Patients Should Know
At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.
Monday, January 19, 2026 – Closed
In observance of Martin Luther King Jr. Day.

Perhaps no disease has garnered more attention in the past couple of decades than breast cancer, which is very gratifying to me as a breast cancer surgeon and specialist.
The pink ribbon and color pink as symbols of breast cancer awareness are everywhere, from automobile dealers to NFL linebackers wearing their pink shoes in October, which is Breast Cancer Awareness Month. Since 1982, the Susan G. Komen organization has promoted breast cancer awareness with fundraising walks and runs all over the country, investing $2.9 billion to date in research, outreach and advocacy.
About 3.5 million women in the United States have a history of breast cancer. In the year 2000, we turned an important corner, with breast cancer cases beginning to decrease and continuing. Deaths due to breast cancer are decreasing at a rate of about 1.3% per year, attributable to improved treatment and earlier detection due to screening.
That’s all good news. But even though people are becoming much more aware of breast cancer and taking individual actions, it still comes with common questions and misconceptions. With many women and even some men fearing the disease, I field a lot of questions and know that misinformation about breast cancer and its treatment is definitely out there.
To be smart about trying to avoid breast cancer, knowing how to be properly screened for it and what to expect from treatment if one gets it, people need to have good information. Following are the misconceptions and myths I hear most often and feel are most important to untangle for better breast cancer awareness.
Related Reading: With Breast Cancer, There Are No Dumb Questions
People often think cancer presents as pain, but this is rarely the case. The majority of the time cancer is painless unless it’s very large or in a very sensitive area near nerves, lymph nodes and muscles. For these reasons a woman can have breast cancer with pain. But one also can have advanced breast cancer without ever feeling any pain. This is another reason proper screening is important for early detection.
The first thing I explain to patients is there is a difference between local, regional and whole-body control. Local control pertains to the use of surgical oncology at the breast level, either performing a lumpectomy or mastectomy. Regional control goes beyond the breast into treatment of the lymph node(s). Whole body or systemic control is the use of additional treatments like chemotherapy and medicines such as targeted therapy and immunotherapy to prevent metastatic disease.
Surgery like a mastectomy or lumpectomy treats the local disease but doesn’t prevent cancer from coming back elsewhere in the body. Even with a small tumor, there is a chance of recurrence. Undergoing endocrine therapy or chemotherapy along with a mastectomy or lumpectomy helps reduce the chance of the cancer returning.
Related Reading: Fresno KFSN TV’s story on cCARE breast cancer “warrior” Stephanie Jackson
We prefer to administer chemotherapy upfront in some tumor types to see the tumor’s response in vivo (in the living organism). This can decrease the size of the tumor in the breast or regional lymph nodes, therefore reducing the amount of tissue removed during surgery. If we downsize the tumor, we can offer lumpectomies to more patients, and avoid axillary dissection (removal of 8-20 lymph nodes in the armpit). Performing less invasive surgery limits complications, enhances recovery and lessens the development of lymphedema.
Giving neoadjuvant chemotherapy can also help predict survival. Patients who demonstrate a complete response (tumor melts away with chemotherapy) have a much better prognosis than those who do not respond. This helps us to identify patients who need additional whole-body therapy.
Breast cancer screening evaluates a woman for breast cancer before any signs or symptoms appear, in hope of catching any cancer early when it is more likely to respond to treatment. Early detection saves lives.
When a woman is diagnosed with breast cancer in one breast, she is often under the impression that removing the other, healthy breast will automatically improve her chances of survival. However, survival depends on a tumor’s ability to spread through the body and return. Lumpectomy and radiation have the same survival rate as a mastectomy. Performing a mastectomy does not eliminate that chance of chest wall recurrence.
Prophylactic surgery does not improve survival either, it only can decrease the chance of a second cancer from forming. Unless a patient has a predisposition to breast cancer, it is unlikely that person who was successfully treated for cancer in one breast will later end up with cancer in the other breast, which occurs in less than 5% of cases at 10 to 20 years out.
This does not mean there is never a precedence for this type of procedure. Removal of both breasts is termed a bilateral mastectomy, and removal of both breasts before cancer presents is termed a prophylactic mastectomy. Both can prove preferable for those with specific genetic markers and family history.
Deciding between having a lumpectomy or mastectomy or having one or both breasts removed can be a cosmetic issue depending on the size of the tumor. If the tumor is large or there are multiple abnormalities in the breast, a mastectomy may be required. If the tumor is small, a lumpectomy may be performed where only part of the breast tissue is removed, followed by radiation. If a mastectomy is needed, a woman may decide to have a mastectomy on the opposite side for symmetry.
Although it does not guarantee a woman will not get breast cancer, National Comprehensive Cancer Network (NCCN) guidelines state it is worth it to consider having a bilateral prophylactic mastectomy if the woman carries a BRCA or CHEK2 mutation. While early and frequent screening may still be a preferred measure for some women in this situation, for other women this can be stressful if they are high-risk and have to undergo screening every six months with regular biopsies.
Not only can men get breast cancer (lifetime risk is 1 in 833 men), but they can also pass down the genetic markers that cause breast cancer in women. When screening for BRCA on the father’s side, we look for high-grade prostate cancer, ovarian cancer (also cancer of the fallopian tube) and pancreatic cancer. We also want to know if anyone on your father’s side has been diagnosed with cancer.
We want to let people know they should still come in to get their mammogram during the pandemic. Although we can’t speak for other cancer clinics, safety procedures have been implemented at our cCARE facilities. The risk of getting COVID-19 in our clinic is much less than your risk of getting it at the grocery store. If you are due for screening, please don’t avoid it due to COVID-19.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.
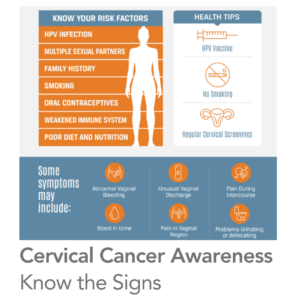
In early stages, cervical cancer may not cause noticeable symptoms. As it progresses, some signs may include: