
Compassionate Care at cCARE: What Patients Should Know
At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.
Monday, January 19, 2026 – Closed
In observance of Martin Luther King Jr. Day.
Aside from skin cancer, breast cancer is the most common cancer found in American women. According to the American Cancer Society, each woman has a 1 in 8 chance she will develop breast cancer within her lifetime. Approximately 1 in 39 women will die from breast cancer. With these high statistics, it is important that women know the basics about breast cancer signs, screening and treatments.
As with any cancer, early detection is key to less treatment and better quality of life. Although it is important to conduct self-screenings and pay attention to any change in look, feel and discharge, we want to find your cancer before you can feel it. The best way to do that is by getting your mammogram.
Patients, family members and fellow physicians have all asked me when they should begin receiving mammograms. This question is difficult because the different medical societies don’t agree. It depends on why you are screening and what your likelihood is of getting cancer.
Breast cancer screening evaluates a woman for breast cancer before any signs or symptoms appear, in hope of catching any cancer early when it is more likely to respond to treatment. Early detection saves lives.
Generally, national screening guideline recommendations are made by looking at survival rate and comparing it to the cost of screening and false positives, not how many lives mammograms can save. This has led to the suggested age range of 50 to 74 (on average, 10 years before end of life) for mammogram screenings, with mammograms every other year.
However, if you look at the American Society of Breast Surgeon’s guidelines and the National Comprehensive Cancer Network (NCCN) guidelines, they recommend mammograms starting at age 40 because there’s a 15% increase in survival if cancer is found earlier. With earlier testing there are more false positives (showing cancer that is actually not there), which requires callback imaging and biopsies that end up negative. These false positives are due to denser breast tissue found in younger women.
We see this give-and-take and try to balance early detection with the cost and stress of false positives. To do that effectively, we often need to individualize screening guidelines.
Related Reading: Navigating mammogram guidelines
I suggest you learn more about your family history of cancer and genetics in order to properly assess your individual threat. This will tell you how diligent you should be in checking for breast cancer signs, and how early and often you should get your mammogram. Although the genetic testing will have to be performed by a professional clinician, you can do your part by learning about your first-degree relatives’ genetic predispositions. First-degree relatives include your mother, sisters, grandparents and daughters.
If you are in any of the following situations, you are at higher risk and should consider beginning screenings at a younger age and having mammograms annually instead of every two years.
Breast cancer treatment plans are as unique as the person being treated. Don’t compare your treatment to others who have had cancer. Do ensure, however, that you have a trustworthy and multidisciplinary team that can come at your cancer from all angles and find the best treatment plan for you.
We have made giant strides in breast cancer treatment. In the past, surgery for breast cancer would remove much larger amounts of tissue, including the chest wall muscle, skin and all lymph nodes above and below the clavicle. This technique left women maimed and in great discomfort.
Now we can give neoadjuvant chemotherapy to shrink the tumor to nearly nothing, allowing us to perform a lumpectomy (removal of a tumor and surrounding tissue only) instead of a mastectomy (removal of the breast). When a patient does need a mastectomy, we now offer reconstruction and can sometimes even save the nipple.
It’s important to remember you shouldn’t avoid certain treatments just because someone you know underwent the same treatment and experienced side effects. Every person’s body is different, and this doesn’t mean you are sure to have side effects as well.
Related Reading: Dr. Bessudo Weighs in on New Breast Cancer Research
The primary treatment methods for breast cancer are surgery, radiation, chemotherapy, antihormone therapy and targeted therapy. These may be used in combination.
Here I want to focus on ways to avoid, manage and heal from some of the side effects of breast cancer treatment from a surgical perspective. There are several steps you can take to make treatment and recovery much more comfortable.
When it comes to radiation, I give patients two pieces of advice. Stretch and use lotion. Radiation is like taking a rubber band and setting it out in the sun: your tissue becomes very tight. Incorporating stretching into your daily activities can help return your tissues to normal elasticity. Swimming and yoga are great exercises to try, or you can stick with simple stretching. No matter how you decide to stretch, do it reliably.
Before and after radiation, treat your skin to a good, thick lotion like cocoa butter with vitamin E. Imagine you are treating a sunburn, as that is essentially how radiation affects the skin. The more you moisturize, the better your skin will look and feel, immediately and years later. Stiffening of the skin from radiation can occur six months to a year after the actual treatment, so what you do right after treatment affects how you look and feel later.
Another possible side effect of breast cancer treatment is lymphedema. This occurs when there is a disruption of the lymphatics of the arm during a dissection underneath the armpit. Lymphedema shows up in about 5% of patients who undergo a sentinel lymph node procedure, which is removal of one to three lymph nodes. The chance of lymphedema is as high as 20%-40% when you remove more of the lymph nodes with an axillary dissection and/or add radiation to the axilla lymph nodes.
Look for signs of swelling in the hand and arm as well as the feeling of heaviness. Seek treatment right away if you see these symptoms. Treatment may include lymph drainage or a compression sleeve.
While proper cancer treatment and management of the side effects from this treatment are very important, it is equally important to make proper lifestyle changes to avoid the return of breast cancer. Here are a few things you can do to improve your overall health and help prevent recurrence.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.
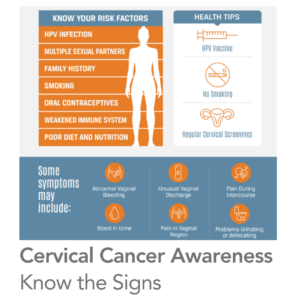
In early stages, cervical cancer may not cause noticeable symptoms. As it progresses, some signs may include: