
Compassionate Care at cCARE: What Patients Should Know
At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.
Monday, January 19, 2026 – Closed
In observance of Martin Luther King Jr. Day.

Although bladder cancer is the seventh most common type of cancer found in the United States, I know from talking with my patients and their family members that it can be one of the most misunderstood as well. Many of the symptoms of bladder cancer, which develops when the cells in the bladder’s lining begin to grow out of control, are similar to symptoms of other medical conditions. This can cause people to overlook bladder cancer as a possibility.
The most common symptoms are blood in the urine, discomfort while urinating, frequent urination, inability to urinate and urinary urgency. These are also symptoms often experienced with a urinary tract infection. Women may attribute blood in the urine to menstruation or spotting as well.
These factors make it difficult to differentiate between a simple infection and a much more dangerous cancer. This is why we urge anyone experiencing any of these symptoms to see their primary care doctor right away.
Lower back pain, fatigue, unintentional weight loss, bone pain and swollen feet can also indicate the disease is in an advanced state. It is especially important for the elderly to seek medical attention if they experience tea-colored urine or visible blood in their urine as they are the most likely to experience this type of cancer, with the average diagnosis age being 73. Most of the cancer patients I see are over age 55 as 9 out of 10 cases of the disease are in this age group.
Although this cancer can cause pain, it is often painless in the early stages of the disease. The blood in the urine can also be microscopic and go unnoticed by the naked eye. Because bladder cancer can have so few obvious symptoms, it is critical to pay attention to all changes in your body.
Don’t wait for pain before visiting the doctor. If bladder cancer is present, the sooner it is detected and treated the better the survivability rate.
A doctor can order a urine test that will show any signs of blood in the urine. Doctors can also test for urinary tract infections. If all benign causes of urinary symptoms have been ruled out, it is time to see a specialist and get tested for bladder cancer.
Unlike several other cancers, there are no recommended screenings for bladder cancer. This type of cancer is typically only found after symptoms arise. cCARE or a urologist can perform several tests for this cancer.
These include a urine test called a urine cytology, a cystoscopy where a camera is inserted into the urethra, and a biopsy of the bladder. A CT scan would be used after a bladder cancer diagnosis to better gauge the extent of the disease.
Treatment methods depend on how advanced the cancer is and the wishes of the patient. It is either considered non-muscle invasive, meaning it is still in the early stage, or muscle invasive, meaning it has spread far into the bladder’s muscular wall or even into other organs and/or the lymph nodes.
Non-muscle invasive bladder cancer (NMIBC) is typically treated by a urologist using techniques that work directly in the bladder, such as intravesical therapy. This therapy administers liquid medication into the bladder using a catheter. It has a lower chance of damaging healthy cells while treating early-stage bladder cancer.
Muscle invasive bladder cancer (MIBC) can be treated through surgery, chemotherapy or radiation, which is my specialty. Surgery can either be a removal of the cancerous tumor, called transurethral resection of bladder tumor (TURBT), or the partial or complete removal of the bladder itself.
Complete removal of the bladder is called a radical cystectomy. If a patient undergoes a radical cystectomy, he or she will require reconstructive surgery in order to store and release urine. Fortunately, many patients do not have to undergo a radical cystectomy.
Chemotherapy can be delivered intravesically (directly into the bladder), in pill form or through an IV. We perform radiation by directing X-rays toward the cancerous region to destroy cancer cells.
Depending on the patient’s wishes, health and the severity of the bladder cancer, some of these treatment options can also be combined. If a patient is to have a cystectomy, he or she will likely undergo chemotherapy for a number of months before the surgery. Patients with MIBC will always undergo chemotherapy, but then their health and wishes will determine if it is followed up with surgery or radiation.
A urologist would perform the surgical aspects of bladder cancer treatment while the experts at the California Cancer Associates for Research and Excellence (cCARE) would provide chemotherapy and radiation.
When it comes to bladder cancer, cCARE has plenty of good news to share. This is one of the most survivable cancers with an average 5-year survival rate of around 77%. The earlier the cancer’s stage, the higher the chance of survival.
cCARE is proud to offer the advantage of streamlined bladder cancer treatment with both chemotherapy and radiation therapy located under one roof. This allows for improved communications between our doctors, which leads to easier and more convenient care for our patients.
We also communicate with experts outside our team during multidisciplinary tumor boards with Saint Agnes Medical Center. During these boards complex cases are discussed with a team consisting of a radiologist, pathologist, medical oncologist and relevant surgeon. These experts review the information gathered on the case, including slides and biopsies, and brainstorm the best treatment plan for the patient.
The best news we can share is there has been great advancement in bladder cancer treatment options. New radiation techniques have allowed for shorter treatment cycles. Where previous radiation would last 7 to 8 weeks, the same treatment can now be administered in only 4 to 5 weeks.
We have also learned how to better spare nearby organs during radiation therapy. New immunotherapy treatments have created the opportunity for improved outcomes, supporting or stimulating the body’s own immune system to fight against the cancer.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.
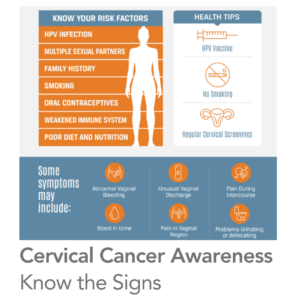
In early stages, cervical cancer may not cause noticeable symptoms. As it progresses, some signs may include: