
Compassionate Care at cCARE: What Patients Should Know
At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.
Monday, January 19, 2026 – Closed
In observance of Martin Luther King Jr. Day.

Whether it’s a friend, family member or yourself going through cancer treatment, many of us have been impacted by pain associated with the disease and its treatment. With about 50% of cancer patients reporting pain as a symptom early in the diagnosis and more than 75% in later stages, pain caused by cancer and its treatment can become difficult to bear and can cause a variety of negative effects such as depression, hopelessness and loss of appetite.
To manage this pain, patients can take narcotic pain medications, also known as opioids. However, there are many downsides to taking oral narcotics.
Related Reading: Managing Weight Loss or Gain Side Effects of Cancer Treatment
The good news is there are other options. One alternative to treating cancer pain with oral opioids is a device called an intrathecal pain pump. This pump continuously administers a small dose of pain medication directly into the spine where pain receptors are present.
The hockey-puck-sized device contains a battery-operated pump and a reservoir of medication. This portion of the device lies near the waist and is connected to a small catheter that is inserted into the fluid-filled intrathecal area surrounding the spine in the back that allows for continuous infusion of medication into the spine. The entire device is surgically implanted underneath the skin.
The pain pump can mitigate many side effects for patients who take opioids orally to manage their cancer pain. This is because only a fraction of the dose of the pain medication is needed since the pump directly introduces the drug to the pain receptors, bypassing the gut. The difference in dose alone offers many advantages.
Side effects such as constipation, fatigue, nausea and vomiting are common with oral medications, but the lower dose used by a pain pump can reduce the severity and frequency of these associated side effects. Morphine is the most common drug used, but we can also use other narcotics such as fentanyl, Dilaudid (generic hydromorphone), or even nonnarcotics such as bupivacaine, clonidine and others if the side effects of one drug are too difficult.
Effective pain management requires correct timing and dosage of the medication. The intrathecal pump eliminates the need for the patient to remember that information, as the device is programmed to deliver medication at a prescribed dose and rate. So, patients never have to worry about when their last dose was received.
Pain varies in severity. In this case, the pain pump offers a better response to breakthrough pain than that of oral medication. If a patient is experiencing breakthrough pain, which is a sudden increase in pain, they are able to press a button on an external device that then signals the pump to release medication at a higher dose to rapidly alleviate the unexpected spike in discomfort.
Patients who use a pill have to wait in pain much longer while their medication takes effect. Since the opioid is constantly being given, pain relief is also more consistent.
The significance of this method is that pain is treated more conveniently and effectively. Therefore, intrathecal pain pumps can significantly improve quality of life, and an increase in survivability for oncology patients using pain pumps has also been recorded. Some studies also indicate that the use of intrathecal drug administration costs less after 3-6 months than conventional forms of treatment using oral pain medications.
However, this option is not perfect.
Surgical implantation of the device is required and complete recovery can take 2-4 weeks. There are also risks associated with the surgery, the most common being infection, cerebral spinal fluid leaks, pump malfunctions (the most common reason for repeat surgery) or overdosing with pain medications. The device may also shift after being implanted and cause discomfort, requiring revision surgery.
Refills of medication every three months are also needed and performed using a small needle under local anesthetic in the physician’s office. Additionally, the batteries last approximately seven years and the pump will then need to be replaced. However, the procedure is simple and recovery is quick.
A recent study showed complications requiring surgery occurred in less than 10% of device implantation cases. Adverse drug reactions may occur but tend to subside as time progresses. Addiction to narcotic medications is a fear that many patients face. While this is one downside of treatment, we need to distinguish between addiction and physical dependence.
Addiction is the compulsive use of a drug in the face of damaging consequences. Physical dependence on a drug means the body adapts to it and requires more of the drug to attain the desired effect. The pain caused by cancer and its treatment can be so debilitating that dependence, not addiction, to narcotic medication must be achieved in order for a patient to enjoy and live life.
Despite these downsides, one study showed that 86% of patients who used intrathecal pain pumps for excruciating pain state they would choose this option again, given the same result. Many other studies also attest to the efficacy of intrathecal therapy with patients consistently reporting high rates of satisfaction, reduction in disability and an increase in quality of life.
Fighting cancer is a battle in itself, and better management of related pain through intrathecal drug therapy can dramatically improve a patient’s quality of life, making their battle against cancer much easier.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.
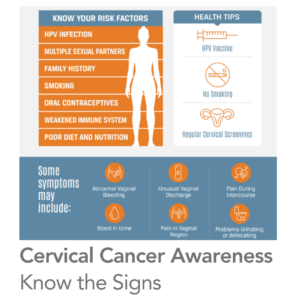
In early stages, cervical cancer may not cause noticeable symptoms. As it progresses, some signs may include: