
Compassionate Care at cCARE: What Patients Should Know
At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.
Monday, January 19, 2026 – Closed
In observance of Martin Luther King Jr. Day.

Palliative care is a lot of things, but “end of life” care it is not. At its roots, it is care to keep living.
Whereas hospice focuses on the last months of someone’s life, palliative care is concurrent with a patient’s illness – ideally, starting at initial diagnosis through any treatment or post-treatment adjustments.
Serious illnesses cause serious, almost unfathomable disruption across a person’s life. The goal of palliative care is to holistically address issues affecting quality of life and improve patient comfort. This can mean tackling someone’s emotional, financial, psychological, social and physical well-being.
In addition, palliative care also emphasizes planning. This can include the choices for medical treatment, organizing medication, juggling family or health visits, writing wills, tackling finances and all the other small or large details that should be pinned down. These conversations and details are daunting in the best of times, let alone when battling an illness. Working with trained professionals to plan for and confront these issues relieves many burdens.
Palliative care is for anyone living an “adjusted life.” It is for people of any age. It is provided on an ongoing basis or for a short period of time, depending on the individual’s needs. Perhaps most importantly, it places an emphasis on the patient, and not the disease, as the primary focus of care.
Harnessed to its fullest, it can bring hope, a sense of control, and a chance at a better quality of life for patients and their caregivers.
cCARE is unique in that it provides palliative care, complementary medicine and cancer support services directly to our patients. Our doctors guide patients through their diagnosis, symptoms and palliative care options from the get-go, cutting down side effects, improving outcomes and decreasing hospital stays.
Our complete services
I mentioned earlier that palliative care should be a part of the care from the onset of the diagnosis of a serious illness. This is based on growing evidence of the positive impact of this care on quality of life.
Most notably, a landmark New England Journal of Medicine study found that early palliative care not only improved quality of life and symptoms of anxiety and depression, but also improved survival in patients with lung cancer.
The connection to quality of life cannot be understated. Medical science enables all of us to live longer lives, which also means our population is getting older and sicker. If my patients have taught me anything, it is that the quality of those days does matter.
As a result, palliative care can look very different from patient to patient.
For a patient with cancer, for example, an oncologist could collaborate with a team to harness a home health aide to provide support to the family or a nurse practitioner to incorporate ways to manage the nausea, loss of appetite or pain that comes with treatment. It could also mean working with community resources to address the financial stress of being too sick to work or the social isolation that can come from missing out on typical activities.
This focused care helps patients feel better, both physically and mentally.
Related Reading: Treatment & Hope Prolong Carole’s Life
Working as a palliative care physician is a great responsibility, but the truth is it also saved me.
A part of who I am as a person and doctor is my desire to relieve suffering. As a young doctor, I grappled with the feeling that I was somehow failing my patients, as they weren’t getting treatment once they were discharged from the hospital. I hated to think they were suffering.
That changed when I discovered the field of palliative care. It was a gift that keeps giving.
I’ve learned about courage and resilience from my patients, and I like to think I have helped them live better lives.
I am grateful for the palliative care movement, and the ability to help patients not only with the quantity of their days but the quality of them as well.
So, now that I’ve dispelled some of the myths and shed more light on what this kind of care is, I hope more patients will consider it.
While the greatest benefits are reaped when care is begun early after the diagnosis of serious illness, it’s never too late to start.
If it hasn’t been offered to you, ask for it. If palliative services are not available locally, your doctor may explore your palliative or hospice needs with you directly. At cCARE, we are proud to provide not only palliative care to our patients, but a wealth of integrated medicine options, community resources and cancer support services.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.

At cCARE, we are proud to provide trusted cancer care in our community. May is a time for awareness, education, and prevention. Learn more about our approach by reading our latest blog.

Follow-up appointments are an important part of staying healthy. Whether you’re managing a condition, monitoring progress, or simply keeping up with routine care, these visits help your healthcare team make sure everything is on track.

Cancer treatment can bring physical, emotional, and mental challenges. Feeling stressed or overwhelmed is completely normal, but there are simple, effective ways to help manage stress and maintain a sense of control during this time.
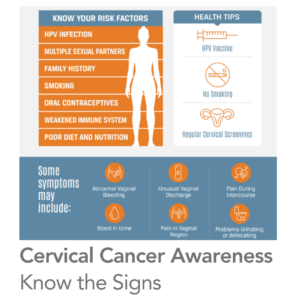
In early stages, cervical cancer may not cause noticeable symptoms. As it progresses, some signs may include: